Bedsores, sometimes called pressure sores or decubitus ulcers, can develop in people who have been confined to bed for long periods of time, are unable to move for short periods of time, or who use a wheelchair or sit in one spot for long periods of time. Other complications, such as aging, circulation and decreased sensation, can increase the likelihood that a person will develop bedsores. Hospital patients and nursing home residents, as well as those who are being cared for at home and who are confined to bed are most at risk to develop bedsores.
Pressure sores develop when one has prolonged immobility which can be due to injury or chronic illness. Once the pressure sore has started to involve the muscle and underlying bone, then it require surgical intervention. Surgical intervention often involves not only the removal of the affected tissue and bone, but then the defect left must be covered with healthy tissue. Some options that we provide include:
- local gluteal skin-muscle and/or skin flap,
- biceps femoris muscle-skin flap,
- gracilis muscle-skin flap, and
- tensor fascia lata muscle-skin flap
In their early stages, bedsores can be treated non-surgically. Left untreated they can lead to dangerous medical complications like bone and blood infections or bacterial infections in a joint.
If the pressure sore has progressed to the point that the ulcer has gone deeper than the skin surface and is affecting bone and tendon, surgery may be the best treatment. The reconstructive surgeons at our clinic can diagnose the problem and recommend appropriate reconstruction.
Because injury and chronic illness often cause the immobility causing pressure sores, there are many factors that need to be addressed to optimize the outcome of these patients.
- Nutrition must be addressed to assure that the patient is taking in a well rounded diet with optimal protein intake.
- Also, many injuries that cause one to be immobile can make a patient have contractures and spasms it is important for these patients to be seen by Neurology and Orthopedics to minimize these factors.
- Proper positioning is vital in these patients so one may need to update and replace cushions for wheelchairs and to replace their mattress with an air mattress.
- Active involvement with Physical Therapy is necessary to help patients position themselves properly, learn good transfer methods to avoid sheering forces, and to help them combat the effects of long immobilization.
- Often these wounds can be infected, so Infectious Disease Service may become involved with the patient care.
- Additionally, patients must be compliant with wound care orders and may find assistance with education from our Wound Care Nurses while in the hospital.
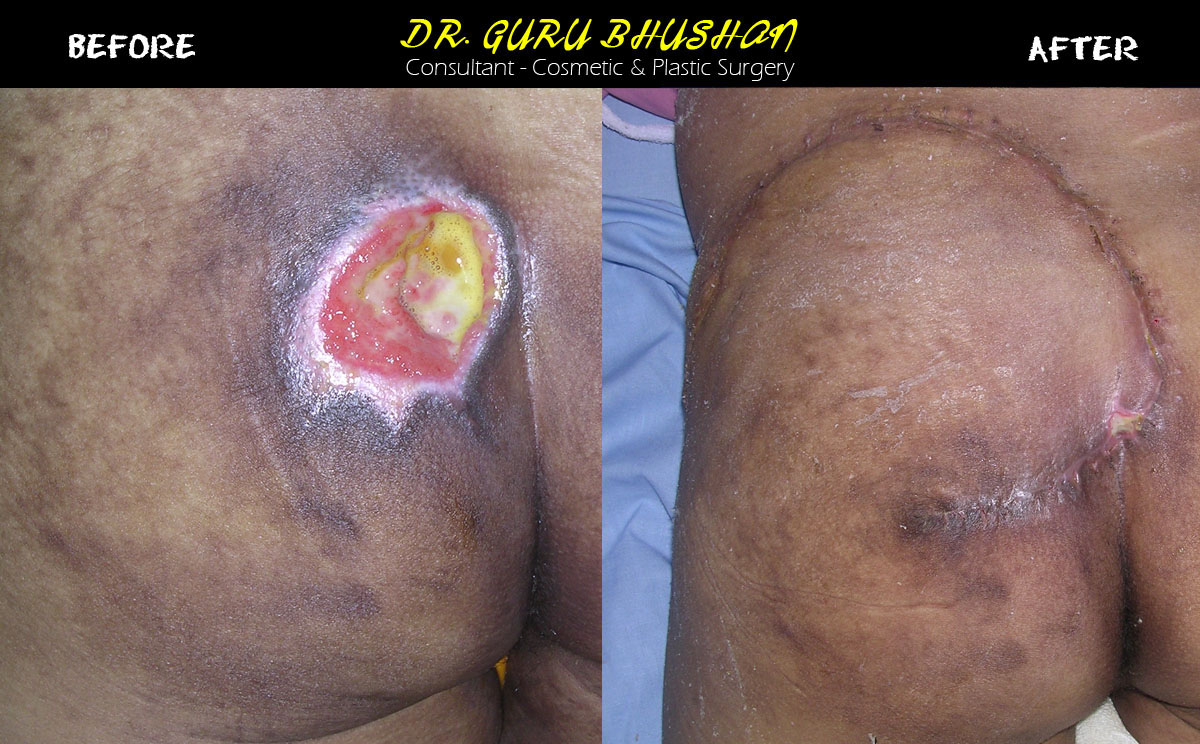
Before/After Picture(s):
Important: "To Enlarge", please click anywhere on the image and "To Close" the larger view, click outside the image or press the 'Escape' key.